What is Genetic Testing for Pregnancy?
Genetic testing for pregnancy or prenatal testing can offer a lot of insight into the genetic material of a fetus and the possibility of birth defects. If there’s a positive result for specific genetic conditions, optimal medical support can be provided to the family. There are several different types of prenatal testing depending on how far along the mother is and which genetic condition is in question (2).
Screening vs Testing
There are two types of prenatal testing: screening and diagnostic testing.
Screening tests identify women who have an increased risk of birthing a child with certain chromosome abnormalities (2). They do not identify specific birth defects or genetic conditions (2). If a woman has a positive result from one of these screening tests she is offered diagnostic testing as the next step. Sometimes screening tests result in a “false positive”. This is when a screening test shows a positive result for a genetic disorder but then the diagnostic test comes back negative (7).
Diagnostic tests are more definitive and can tell genetic counselors if a baby has a certain genetic abnormality. They can be performed during a first-trimester screening or during the second trimester (2). Diagnostic testing is presented in two forms:
- Chorionic villus sampling (CVS): A doctor must gather a tissue sample from the placenta by inserting a needle into the woman’s abdomen or inserting a catheter into the cervix. It is performed between 10.5 and 13.5 weeks of pregnancy (2).
- Amniocentesis: This procedure requires a doctor to insert a small needle into the mother’s abdomen to obtain a sample of amniotic fluid (2).
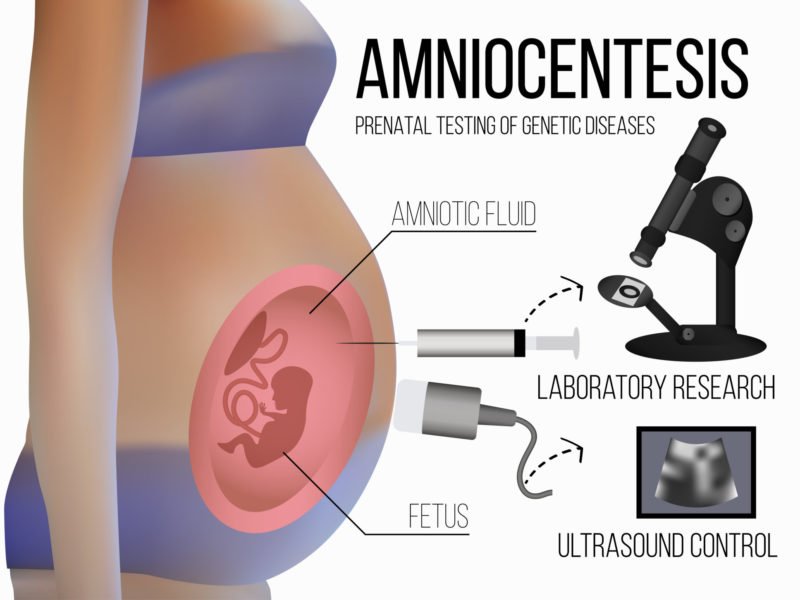
The cells gathered from the above procedures are then used for the genetic testing. The time it takes to receive results is dependent on the type of genetic test ordered.
There is a very small risk of miscarriage in performing both CVS and amniocentesis. For CVS there is a 0.5%-1.0% chance of miscarriage, and for amniocentesis, there is a 0.25%-0.50% chance (19). Benefits and risks of each procedure should be deeply explored before committing to a prenatal test. The chances of parents passing disease to their children should also be discussed.
Non-Invasive Prenatal Testing
During pregnancy, a woman and her partner may choose to take a blood test in order to see if the unborn baby has an increased risk for genetic conditions. Prenatal testing used to be a very invasive process, but due to new DNA sequencing technologies, it can now be done by using a small sample of the mother’s blood. There are slight amounts of fetal DNA in the mother’s blood, and by testing this blood a genetic counselor can detect specific genetic disorders in an unborn child (1). This process is known as cell-free DNA testing or non-invasive prenatal testing. It is a form of first-trimester prenatal screening. Screening determines the risk factors for genetic problems.
Prenatal testing and genetic counseling before birth can help with early diagnosis. Some of the most common genetic conditions tested for during prenatal testing are Cystic Fibrosis, Sickle Cell Disease, and Tay-Sachs disease (8).
Cystic fibrosis is a life-threatening condition that can affect the lungs and cannot be cured but eased with treatment (9). Sickle Cell Disease causes an irregular shape of red blood cells and is another genetic condition that cannot be cured, but with proper treatment, there is an ease in symptoms (10). Tay-Sachs Disease is a very rare genetic condition that severely alters a person’s quality of life (11). Early treatment for Tay-Sachs Disease and the other genetic disorders mentioned ensures the highest quality of life for these patients.
Who Should Consider Prenatal Diagnostic Tests?
Pregnant women who have a family history of genetic conditions should especially consider genetic screening tests. However, the most common reason pregnant women undergo prenatal genetic testing is due to age (2). The chance of having a baby with a genetic disorder increases as a woman ages. Other reasons expecting mothers opt for testing may be due to unusual ultrasound results or if a parent is a suspected carrier for a genetic disorder (2).
At age 35 and above there is an increased risk of genetic disorders (12). Genetic testing for pregnancy over 35 is highly recommended. A woman who conceives at age 25 has a 1 in 1,250 chance of birthing a child with Down Syndrome compared with a woman conceiving at age 40 who has a 1 in 100 chance (12). While 35 is considered advanced maternal age, women above the age of 30 should thoroughly discuss their pregnancy health with their doctors (12). Chromosome abnormalities increase, and so does the risk of miscarriage, as a woman ages (12).
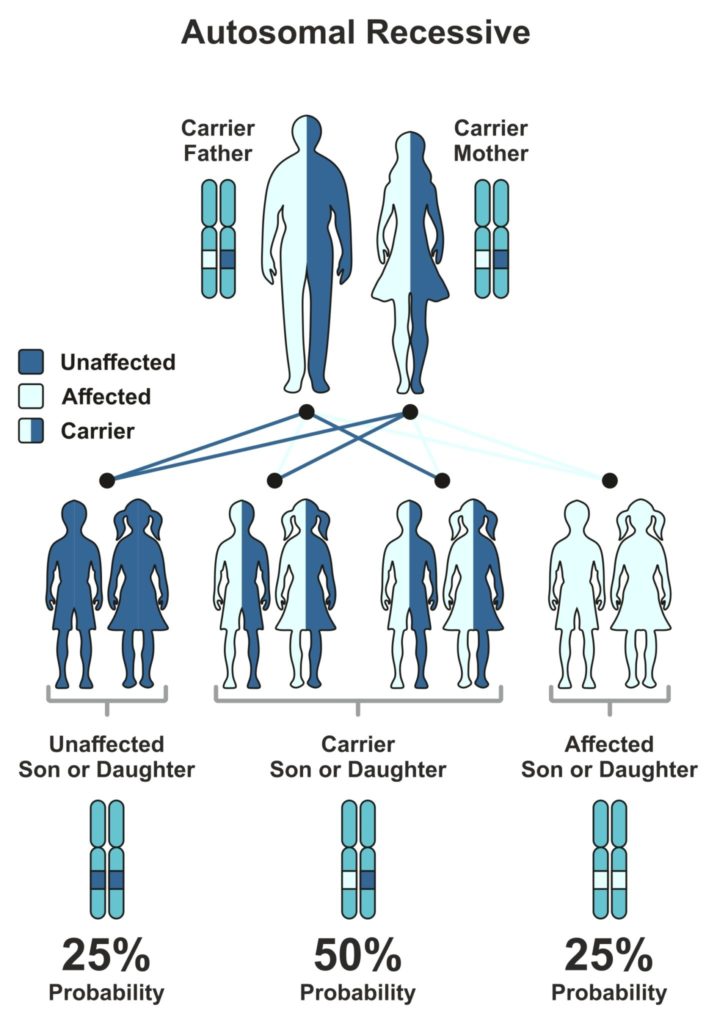
Cystic Fibrosis, Sickle Cell Disease, and Tay-Sachs Disease are all inherited through an autosomal recessive pattern. Autosomal recessive means two copies of a gene must be mutated in order to have a disorder (13). These diseases are typically passed on by two carriers. A carrier is a person who holds a trait for a genetic disease but does not have the disease. If both parents are carriers for a disease there is a 25% chance their child will possess the disease (14).
Cost of Prenatal Testing
The cost of non-invasive prenatal testing in the United States ranges from $800 to $2000 (16). Most of the time insurance plans will cover prenatal testing if it is recommended by a doctor. Oftentimes first-trimester screening and second-trimester screening are covered by health insurance plans. Some even include diagnostic tests like chorionic villus sampling. There is a government program called WIC (women, infants, and children) in every state that can help a woman if she is unable to pay for preventative prenatal care such as genetic screening (15). WIC also provides nutritional counseling (15).
Benefits of Genetic Testing for Pregnancy
There are a lot of positives to knowing the genetic information of a fetus. For example, Down Syndrome children have a much higher risk for heart defects. If the expecting parents and their healthcare professionals are aware of this they can assemble the proper pediatric team to perform surgery after birth. Parents can also prepare themselves for raising a child with special needs (1).
Prenatal testing can provide insight into a child’s future healthcare needs. It can detect neural tube defects and life-threatening diseases such as Tay-Sachs Diseases and Cystic Fibrosis. Neural tube defects are birth defects of the brain, spine, or spinal cord (5). Spina Bifida is a neural tube defect where the spinal cord doesn’t develop correctly (5). Folic acid (a common vitamin found in most multivitamins) can prevent Spina Bifida, and therefore mother’s at increased risk should consume the proper amount folic acid (6).
It is very important to maintain a well-balanced diet containing lots of vitamins to ensure a baby develops properly. Nutrigenomics looks at the interaction of genes and nutrition, especially in relation to how our diet affects disease risk, prevention, and treatment. A nutrigenomic diet for pregnant women should contain plenty of iron, calcium, and folic acid. Calcium promotes bone growth and iron is helpful for the baby’s blood supply (18). Not only does folic acid prevent Spina Bifida, but it also helps protect against other birth defects, such as Anencephaly, by more than 70 percent (17).
Consuming the proper amount of food from each category (grains, meat, fruit, vegetables, and dairy) will give expecting mothers the vitamins and nutrients required for a healthy baby. Mothers should increase their caloric intake during each trimester to guarantee proper fetal development (18). For the average woman, a good rule to follow is 1,800 calories a day for the first trimester, 2,200 in the second, and 2,400 in third (18).
Ethical Concerns Moving Forward
Non-invasive prenatal testing can be performed very early in pregnancy and parents may even choose to terminate a pregnancy if test results show the likelihood of certain birth defects (1). Undoubtedly, this sets the stage for controversial debates in the healthcare world.
Prenatal testing mainly identifies chromosome abnormalities such as trisomy (1). Trisomy is the term used when a person has three copies of a chromosome instead of the normal two. Chromosome abnormalities include trisomy 13 (Patau Syndrome), trisomy 18 (Edward’s Syndrome), and trisomy 21 (Down Syndrome).
Babies born with Patau Syndrome and Edward’s Syndrome suffer severe birth defects and have a very low life-expectancy of less than a month (3)(4). Parents could choose to terminate the pregnancy if they know their baby is going to suffer from these chromosomal conditions. This puts forth an extensive ethical debate over the powers of genetic screening.
Genetic counselors have pointed out that conditions such as Down Syndrome may be completely eliminated from the population if parents choose to terminate these pregnancies. The Nuffield Council for Bioethics fears parents might start using prenatal testing to determine the sex of a baby, and terminate the pregnancy should it not be the gender they want (2).
Just like most technological advances in society, these new advances in genomic medicine bring forth tremendous gains for society. However, with new advancements come new social issues. Genetic testing for pregnancy is beneficial in numerous ways, but meeting with a genetic counselor can help determine if or how precisely someone should pursue genetic testing for their baby.
Citations
- https://www.genome.gov/27570937/april-17-noninvasive-prenatal-genetic-testing/
- https://www.ncbi.nlm.nih.gov/books/NBK115544/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4543265/
- https://ghr.nlm.nih.gov/condition/trisomy-18#inheritance
- https://medlineplus.gov/neuraltubedefects.html
- https://medlineplus.gov/spinabifida.html
- https://ghr.nlm.nih.gov/primer/newbornscreening/nbspositive
- https://www.urmc.rochester.edu/encyclopedia/content.aspx?contenttypeid=85&contentid=p01241
- https://www.nhlbi.nih.gov/health-topics/cystic-fibrosis
- https://www.cdc.gov/ncbddd/sicklecell/index.html
- https://rarediseases.info.nih.gov/diseases/7737/tay-sachs-disease
- https://www.urmc.rochester.edu/encyclopedia/content.aspx?ContentTypeID=90&ContentID=P02481
- https://ghr.nlm.nih.gov/primer/inheritance/inheritancepatterns
- https://medlineplus.gov/ency/article/002052.htm
- https://www.womenshealth.gov/pregnancy/youre-pregnant-now-what/prenatal-care-and-tests
- https://www.ncbi.nlm.nih.gov/books/NBK274056/
- https://www.health.ny.gov/publications/1335/
- https://medlineplus.gov/ency/patientinstructions/000584.htm
- https://www.cdc.gov/mmwr/preview/mmwrhtml/00038393.htm


 Nutrigenomics: Using Nutrition to Lessen Disease Risk
Nutrigenomics: Using Nutrition to Lessen Disease Risk